
A milestone: the first long-term study on two-piece zirconia implants was published. The independent prospective study at Heinrich-Heine-University Düsseldorf examined two-piece Patent™ Implants (Zircon Medical Management AG; formerly ZV3 – Zircon Vision GmbH) after 9 years of function.[1] The results are ground-breaking and close a fundamental gap in research.
Fig. 1: Zircon Medical CEO Marco Waldner (left) unveiled the results of the independent 9-year study together with Patent™ user and implant specialist Prof. Dr. Marcel Wainwright at IDS 2023 in Cologne.
The results after 9 years:
• No peri-implantitis was found
• A high survival rate was documented
• The soft tissues were healthy (bleeding on probing (BOP): 12.9%)
• No implant fractures were reported
• Plaque indices (PI), pocket depths (PD), and bleeding on probing (BOP) were stable at the 2- and the 9-year follow-ups
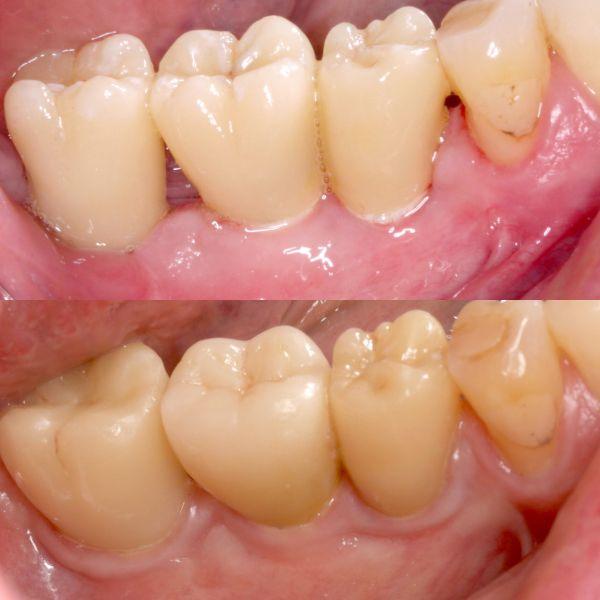
• Clinical improvements of the soft tissues were observed (Fig. 2 on the right: Soft-tissue creep from baseline to 9-year follow-up)
Conclusion: The Patent™ Implants investigated maintained hard- and soft-tissue health and stability over the long term and are therefore confirmed as predictable long-term tooth replacement solution.
What the 9-year study means for implant success
Until now, there have been no long-term observations of two-piece zirconia implants. The implant systems currently available on the market are generally being studied less frequently in long-term studies. Existing studies often limit their observation periods to a maximum of five years. On the one hand, most of the implant systems that have already been scientifically tested over an extended period are no longer available on the market. On the other hand, the introduction of new product lines is advancing so rapidly that scientific evaluations over longer periods of time are nearly impossible.[2] This is concerning since the prevalence of biological complications such as peri-mucositis and peri-implantitis increases over time.[3, 4] Uncontrolled peri-implantitis can lead to infections in the oral cavity, which in turn can put a strain of the immune system and increase the risk of other diseases. Studies indicate that there might be a link between untreated peri-implantitis and chronic diseases such as diabetes, autoimmune diseases and immunodeficiencies such as Crohn’s disease and rheumatic diseases.[5-7]
The ground-breaking 9-year study offers dental professionals and patients a crucial insight:
Long-term oral health can be achieved in a predictable way with the right dental implant system.

Prof. Dr. Jürgen Becker, principal investigator and director of the Department of Oral Surgery at Heinrich-Heine-University in Dusseldorf, commented on the results: ”With our 9-year observation of two-piece zirconia implants we close a fundamental gap in science!”
Thomas Zeltner, Chairman of the WHO Foundation, said on the occasion of an event to present the study results: ”The oral cavity is a crucial key to overall health, quality of life, and healthy aging. The epithelial lining is the Achilles' heel of the human body, so to speak: oral inflammations are associated with chronic diseases such as rheumatism or autoimmune diseases. Prevention is the best form of treatment: that is why we must effectively combat periodontitis and peri-implantitis. The present long-term results demonstrate that this is sustainably possible with dental implants.”

References
1. Brunello G, Rauch N, Becker K, Hakimi AR, Schwarz F, Becker J (2022) Two-piece zirconia implants in the posterior mandible and maxilla: A cohort study with a follow-up period of 9 years. Clinical Oral Implants Research; 33 (12): 1233–1244. DOI: 10.1111/clr.14005
2. Thiem DGE, Stephan D, Kniha K, Kohal RJ, Röhling S, Spies BC, Stimmelmayr M, Grötz KA (2022) German S3 guideline on the use of dental ceramic implants. Int J Implant Dent.;8(1):43. DOI: 10.1186/s40729-022-00445-z
3. Derks J, Tomasi C (2015) Peri-implant health and disease. A systemic review of current epidemiology. Journal of Clinical Periodontology; 42 (16): 158–171. DOI: 10.1111/jcpe.12334
4. Renvert S, Lindahl C, Persson GR (2018) Occurrence of cases with peri-implant mucositis or peri-implantitis in a 21–26 years follow-up study. Journal of Clinical Periodontology, 45 (2): 233–240. DOI: 10.1111/jcpe.12822
5. Naujokat, H (2022) Zahnimplantate bei Diabetes mellitus. S3-Leitlinie (Langfassung), Version 2.0. DGI & DGZMK: Hannover, Düsseldorf. AWMF register: 083-025.
6. Grötz, KA, Duttenhoefer, F, Füssinger, MA, Boeker, M, Beckmann, Y (2019) Dentale Implantate bei Patienten mit Immundefizienz. S3-Leitlinie (Langversion). DGI & DGZMK: Hannover, Düsseldorf. AWMF register: 083-034.
7. Jackowski, J (2018) Zur Problematik oraler Implantate bei rheumatischen Erkrankungen. Available under: https://www.quintessence-publishing.com/deu/en/news/zahnmedizin/implantologie/zur-problematik-oraler-implantate-bei-rheumatischen-erkrankungen






